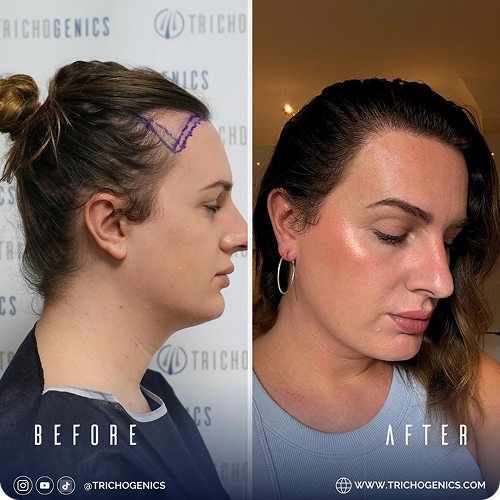
These changes may affect the scalp or other areas of the body, depending on circulation and overall health.
Hair loss from diabetes often improves when blood sugar levels are stabilized through diet, exercise, and medical treatment. Consistent management helps restore follicle function and supports gradual hair regrowth, although recovery may take several months and varies by individual.
In cases where hair shedding becomes long-term or permanent, some individuals explore clinical options such as those discussed at Trichogenics, where techniques like FUE (Follicular Unit Extraction) or DHI (Direct Hair Implantation) are used within a structured medical framework.
Key Takeaways
- Diabetes can damage blood vessels and reduce the delivery of oxygen and nutrients to hair follicles, leading to hair loss.
- People with diabetes may notice thinning, shedding, or patchy loss depending on circulation and immune factors.
- Hair regrowth is possible if the hair growth cycle stabilizes, but recovery often takes months.
- Managing diabetes through lifestyle changes and proper blood sugar control supports better hair outcomes.
- Persistent or unusual hair shedding should be evaluated to rule out conditions like alopecia areata.
How Diabetes Affects Hair Growth
Diabetes can disrupt the hair growth cycle by shifting more follicles into the shedding phase. When blood sugar is not stable, the body, including the scalp, does not function optimally. This can lead to increased shedding and slower replacement over time.
The hair growth cycle includes growth, rest, and shedding phases, and an imbalance among them can lead to hair shedding. High glucose levels can damage blood vessels and reduce the flow of oxygen and nutrients to follicles. This weakens follicle function and contributes to hair thinning.
Types of Diabetes and Hair Loss
People with type 1 and type 2 diabetes can both experience hair changes. The causes differ but often involve circulation issues, immune responses, and metabolic imbalance.
Type 1 diabetes may involve immune system attacks that can trigger alopecia areata, in which the immune system targets hair follicles. Type 2 diabetes is linked to insulin resistance, which can damage blood vessels and reduce follicle support, leading to reduced hair density.
Common Causes of Hair Fall Due to Diabetes
Hair fall due to diabetes often results from a combination of factors. These include poor circulation, stress, hormonal imbalances, and diabetic medications. Each factor can disrupt the hair growth cycle and contribute to reduced hair density.
Chronic high blood sugar can damage blood vessels over time, leading to more persistent hair shedding. This reduces long-term support for follicles and may cause progressive thinning. Early control of glucose levels helps limit these effects.
Some diabetes treatments may also cause hair shedding as a side effect, and certain supplements discussed in glucosamine and shedding effects may also play a role, although this does not occur in all patients.
Treatment options may include topical solutions such as minoxidil (Rogaine), oral options such as hair-support tablets, and lifestyle changes. A medical assessment can help determine if a side effect is contributing to the problem.
What Does Diabetes Hair Loss Look Like
Hair loss in people with diabetes can appear in different ways. Some notice gradual thinning, while others experience sudden shedding or patchy loss, which is commonly linked to immune-mediated attacks or reduced hair on areas like the legs.
Diffuse thinning is common, whereas patchy loss may suggest conditions such as alopecia areata. Many patients also notice more hair on pillows or in the shower, which can indicate changes in the hair growth cycle.
Can Hair Loss From Diabetes Be Reversed?
Hair loss from diabetes can sometimes be reversed, especially when blood sugar levels are well controlled. Stabilizing glucose helps restore normal hair growth cycles and supports follicle recovery. However, results depend on how long the condition has been present and how severe the damage is.
Regrowth may take several months and is often gradual rather than complete. Early-stage hair thinning is more likely to improve than long-term or advanced hair loss.
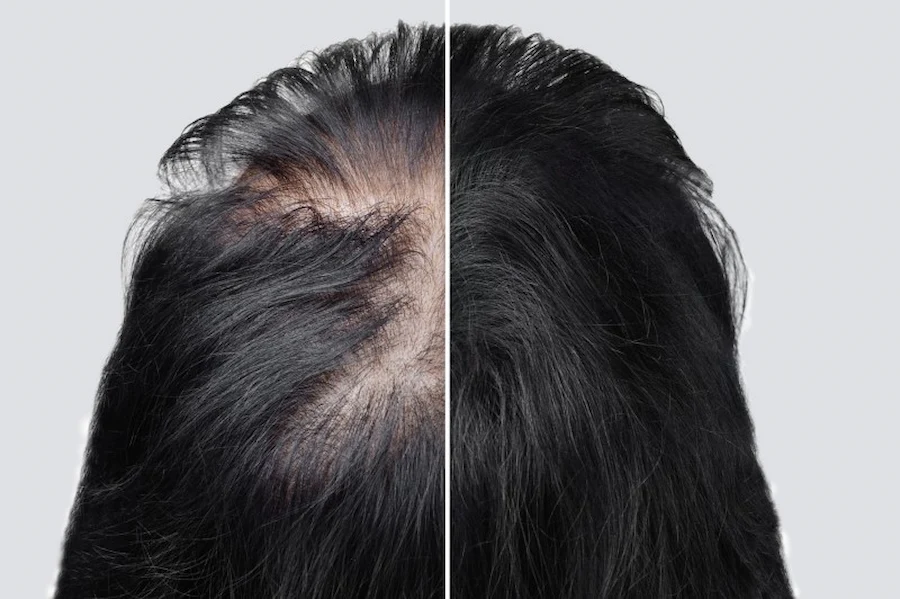
How to Prevent and Stop Hair Loss From Diabetes
Preventing hair shedding focuses on managing diabetes and supporting overall health. Stable glucose levels and consistent blood sugar control help protect blood vessels and follicle function.
In some cases, people ask if diabetes makes you lose your hair because they notice ongoing shedding despite treatment. This often reflects incomplete control or multiple contributing factors rather than a single cause.
Treatment options may include topical solutions such as minoxidil (Rogaine) and lifestyle changes. Diet, exercise, and stress control support circulation and hormonal balance.
How Doctors Diagnose Diabetes Hair Loss
Doctors assess symptoms, medical history, and lab results to determine causes. This evaluation may include reviewing long-term glucose patterns, hormone levels, and signs of immune system activity. Blood tests help evaluate glucose control and other contributing factors.
This helps determine whether diabetes is the primary cause or one of several contributing factors.
When Hair Loss May Signal a Problem
A reduced hair density can indicate poor control or complications in people with diabetes. Certain patterns require attention and evaluation.
- Sudden or excessive shedding
- Hair loss on the legs
- Patchy loss from immune system attacks
- Thinning that continues despite managing diabetes
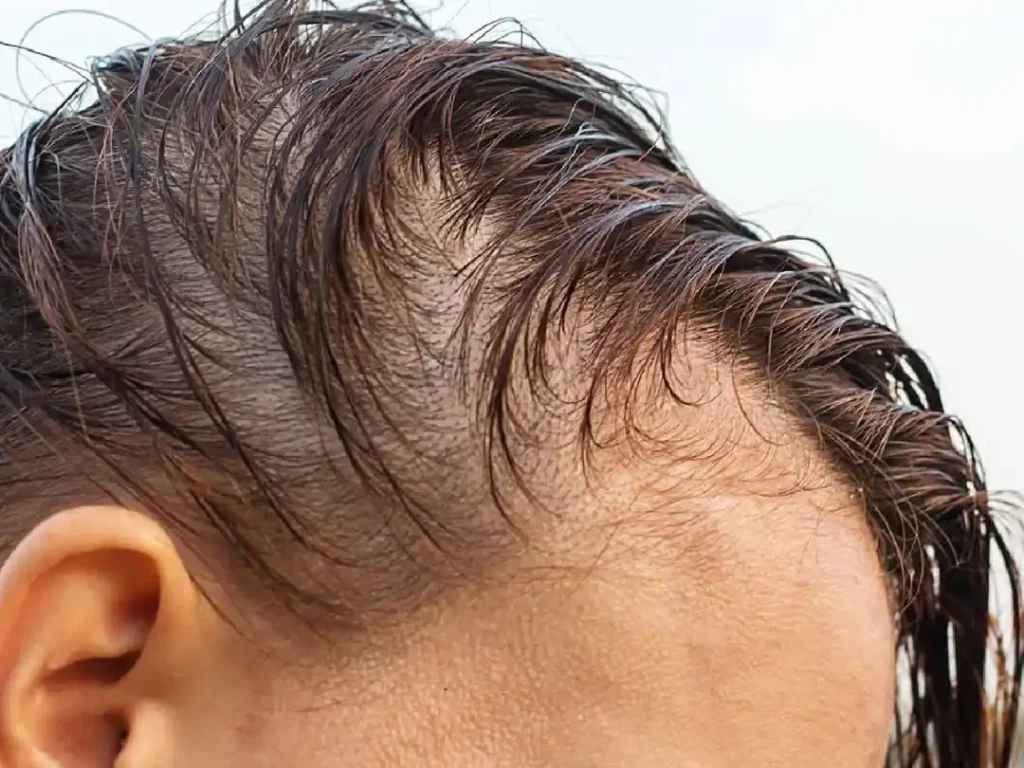
These signs do not always indicate a serious issue, but should be evaluated in context.
When to See a Doctor
You should seek medical advice if hair thinning is persistent, severe, or unusual. Early evaluation helps identify reversible causes and guide treatment. A doctor can assess whether the issue is related to blood sugar levels, hormonal imbalances, or other conditions.
In cases of permanent reduced hair density, some people consider hair restoration procedures, but standards vary by region. Countries like Israel and Greece maintain structured medical oversight compared to less regulated environments abroad.
If you are exploring medical options, you can schedule a consultation with a qualified specialist to review your condition and discuss appropriate next steps.