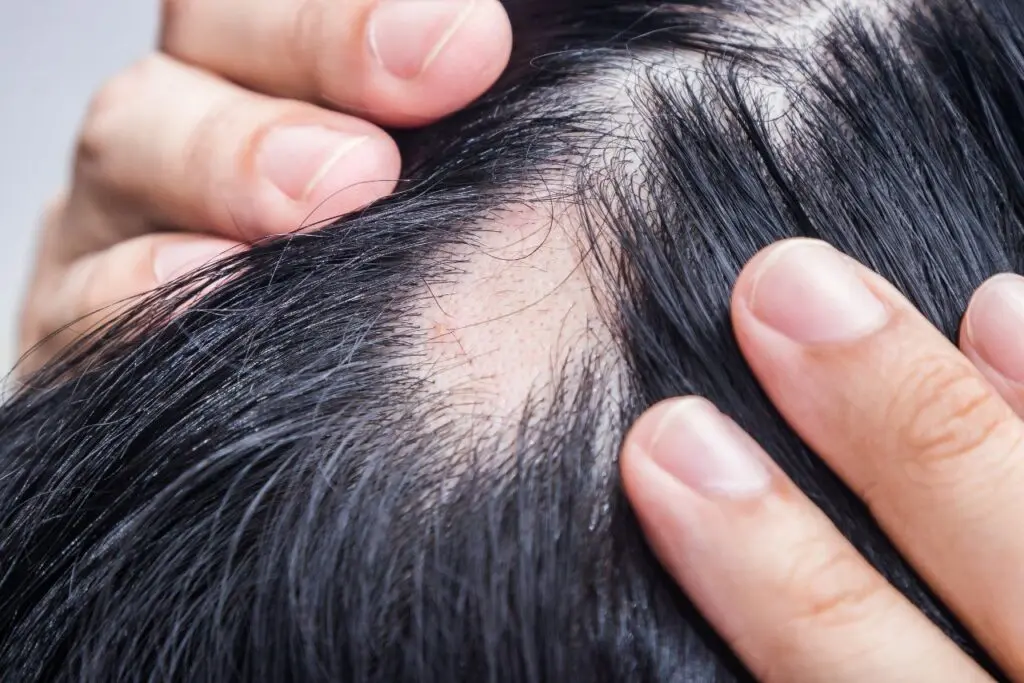
In many cases, hair lost due to autoimmune hair loss can grow back because the follicles remain alive, but regrowth is unpredictable and may occur in cycles of loss and recovery, depending on immune activity.
Hair regrowth depends on how the immune response behaves over time and whether treatment is used to control inflammation around the follicles. Some individuals experience full regrowth within months, while others may have recurring episodes or more persistent loss without scarring.
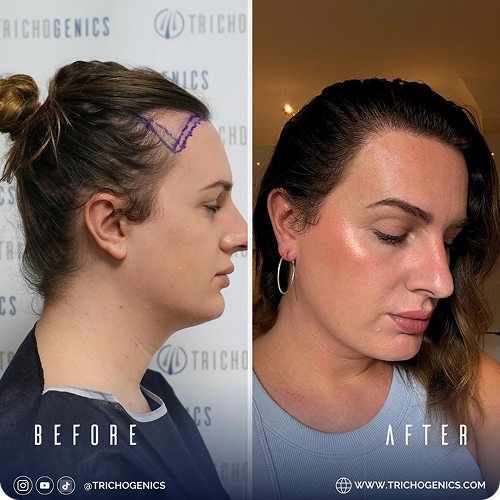
At Trichogenics, with clinics in Greece and Israel, this condition is approached through careful diagnosis and management, as understanding the underlying immune process is key to evaluating treatment options and long-term outcomes.
Key Takeaways
- Autoimmune hair loss occurs when the immune system attacks hair follicles, often leading to patchy hair shedding on the scalp or body, most commonly seen in alopecia areata.
- Hair can grow back if the follicles remain alive, but regrowth is unpredictable and may vary depending on severity, immune activity, and treatment response.
- Diagnosis involves clinical evaluation and may include blood tests to identify underlying autoimmune conditions or related factors such as thyroid disease.
- Treatment options, including corticosteroids, immunotherapy, and newer medications, aim to reduce the immune response, but results can take weeks to months and may include side effects.
- The condition often follows a cycle of hair loss and regrowth, so long-term monitoring and individualized management are important to maintain results and address recurrence.
Autoimmune Hair Loss Causes and Triggers
Autoimmune Diseases That Cause Hair Loss
This occurs when the body misidentifies healthy hair follicles as a threat. This immune response disrupts the hair growth cycle, leading to hair thinning and bald patches.
Common autoimmune disorders include alopecia areata, in which the immune system attacks hair follicles, causing patchy hair shedding. Other conditions, such as thyroid disease and lupus, may also affect the scalp or body, and factors like diabetes-related hair changes can further influence follicle function.
People with alopecia areata may experience cycles of loss and regrowth. The severity ranges from small patches to extensive loss.
Common Triggers and Risk Factors
Triggers such as stress, infections, hormonal changes, and certain medications that affect hair growth can activate the immune response. Genetic predisposition and autoimmune conditions increase risk.
A balanced diet supports overall health but does not directly prevent autoimmune conditions, although issues like vitamin B12 deficiency and its impact on hair may influence overall follicle health.
Autoimmune Hair Shedding Symptoms and Appearance
What Does Autoimmune Hair Loss Look Like
Autoimmune hair shedding often appears as smooth, round bald patches on the scalp, eyebrows, or beard. These areas usually lack redness or scarring. In some cases, diffuse hair thinning may also occur.
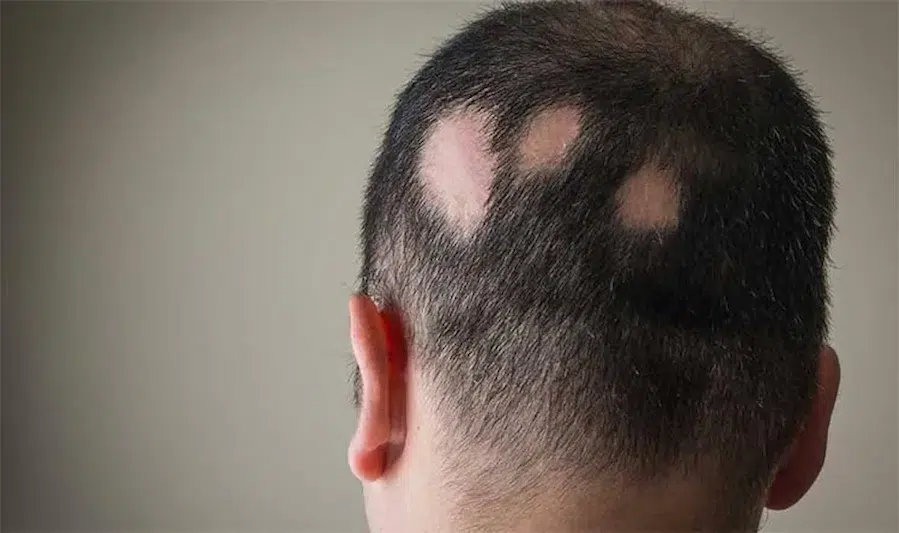
Early Signs and Progression
Early signs include sudden shedding, patch formation, and short, broken hairs. The condition may remain localized or spread. Some individuals experience regrowth, while others develop recurring patterns.
For example, a small patch may regrow within months, while another area develops later, reflecting fluctuating immune activity.
Diagnosis and Blood Tests
Medical Evaluation and History
Doctors evaluate the pattern of the reduced hair density and review the medical history. A scalp exam helps identify key signs such as bald patches or regrowth. This step helps confirm autoimmune-related hair shedding.
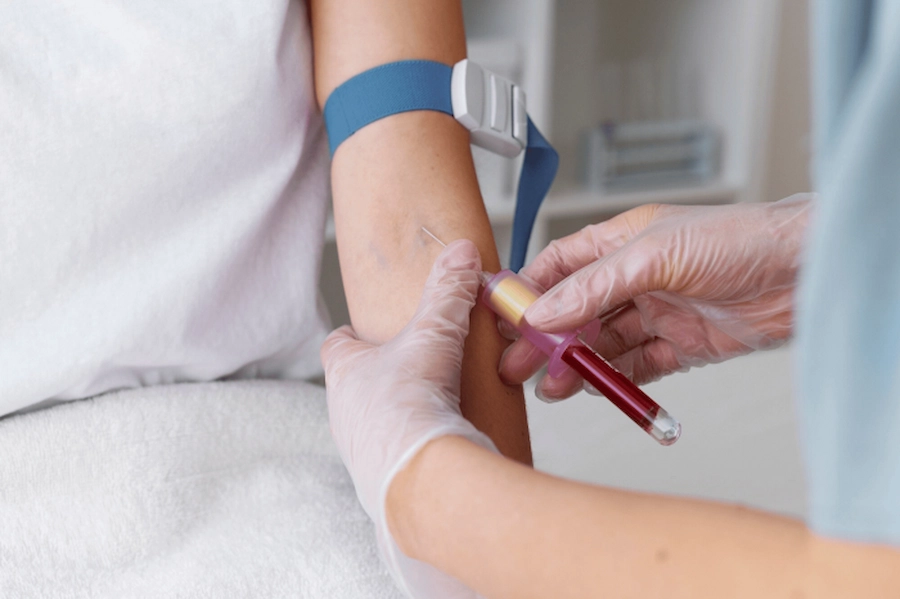
Autoimmune Hair Loss Blood Test
Blood tests help identify underlying autoimmune disorders and rule out other causes. Common tests include thyroid panels and immune markers. These support accurate diagnosis and treatment planning.
Autoimmune Hair Loss Treatment
How to Stop Hair Shedding in Females
Treatment focuses on managing autoimmune conditions affecting hair follicles while supporting regrowth. In females, options include topical treatments and anti-inflammatory medications. Results vary depending on severity.
Medications and Therapies
Treatment options, including corticosteroids, topical immunotherapy, and JAK inhibitors, help reduce immune system attacks. These therapies are used to treat autoimmune responses that interfere with the hair growth cycle. Results may take time and can involve side effects, so medical supervision is important.
Procedures such as FUE (Follicular Unit Extraction) and DHI (Direct Hair Implantation), using tools like the Choi pen, are recognized techniques in modern hair transplant techniques when appropriate. These are doctor-led procedures that require proper evaluation and follow-up.
Initial regrowth may begin within a few weeks, but more consistent results often require several months of treatment. Clinics in Israel and Greece operate under structured medical standards, while some countries, such as Turkey, may have variable regulatory oversight.
Does Autoimmune Hair Loss Grow Back?
Factors That Affect Regrowth
Hair regrowth is possible because the follicles remain alive, even in this form of hair shedding. Outcomes depend on factors such as the severity of the condition, how long the immune system attacks the follicles, and how early treatment begins. Recurrence can occur even after full regrowth, especially in people with ongoing autoimmune activity.
Mild cases with small patches often recover faster, while more extensive forms may require longer treatment and have less predictable outcomes.
Overall health and the presence of other autoimmune conditions can also influence recovery. Some patients recover fully, while others experience slower or incomplete regrowth.
Recurrence and Long-Term Outlook
Autoimmune hair shedding often follows cycles of loss and regrowth, with varying frequency and severity. Some patients may experience a single episode with full recovery, while others develop recurring patches over months or years.
In more persistent cases, the condition can progress to more extensive reductions in hair density, especially if the immune response remains active. Ongoing monitoring helps detect early signs of recurrence and adjust treatment to manage flare-ups more effectively.
How It Differs From Other Hair Loss
Autoimmune hair loss differs from hormonal and stress-related forms. Hormone-reduced hair density is gradual, whereas autoimmune hair shedding occurs suddenly and presents with well-defined bald patches. Stress-related hair loss causes diffuse shedding rather than targeted follicle disruption. Unlike some other conditions, this form of hair loss does not involve permanent damage to the follicles.
If you are experiencing signs of autoimmune hair shedding or ongoing hair thinning, a proper evaluation can help clarify the cause and guide next steps. At Trichogenics, consultations focus on understanding your condition, reviewing treatment options, and setting realistic expectations based on your case.
You can schedule an appointment to discuss your situation and receive a personalized clinical assessment.